Let’s face it. Being a doctor during the pandemic kind of sucks. The past year has presented many challenges in healthcare. From the Covid-19 pandemic to the recent Texas winter storm and power outages, private medical practices have had to pivot and innovate or suffer the consequences.
Pandemics, ice storms, and power outages do not stop pregnancies or those who care for them. Pregnant people need care, and their babies are still coming out. Caring for our patients is goal number one, but we can not do it if Covid-19 or a winter storm keeps the office doors closed.
The Texas storm’s first strike hit the Dallas/Fort Worth region on Thursday, February 11. Our practice made the fast-acting decision to close for inclement weather. We always strive to stay open and operational to the best of our abilities. Still, we closed because the icy roads presented a hazard for our staff and patients.
After Thursday, the practice had to come together and make some tough decisions. The weather reports were getting worse. From everything we read, the following week was going to be an environmental catastrophe. We knew it would be freezing cold with lots of snow, but we had no idea the Texas electric grid would collapse, leaving millions without power or water.
The operations team took preemptive action behind the scenes in a whirlwind of meetings, phone calls, and text messages. We needed a plan to provide safe, effective patient care without putting our staff or patients in danger. The Operations and Clinical teams worked together to ensure the plan was agile and fool-proof.
The first priority was planning for Monday’s snowstorm. We followed our step-by-step operations and communications weather-related playbook. The expected snow, ice, and brutal temperature drops arrived on schedule. What followed was state-wide power outages.
Our plan was to convert most of our visits to Telemedicine. As the morning arrived, many of our providers had no power or Wifi access. Our communications center suffered the same challenges. Using SMS technology, we were able to communicate the rapidly changing plans to our patients. Despite the challenges, we were able to make 7246 rescheduling phone calls and messages.
Two of our physicians moved into a hotel after losing power. At 3:00 am, the hotel lost power and electricity as well. Most of our providers lost water and quickly learned how to flush toilets with snow.
Chief Operations Office Johan Hultman stated, “We had a plan, and we worked the plan. As things progressively got worse, we reworked the plan. We dealt ourselves as many cards to play as we could, and that gave us the ability to maintain control.”
By Wednesday, the weather had somewhat improved. We opened the office late and extended hours to allow patients and staff to drive during daylight. Staff members without power and water came early to shower and brush their teeth. The doctors who could safely make it to our offices saw 752 patients.
The entire team worked together to care for each other. Two physicians with pick-up trucks ran a shuttle service to chauffeur office staff. Other team members took bottles of water to their coworkers.
We did not have enough available medical assistants to staff an entire team. Our providers had to improvise. I moved into the nursing workstation to check vital signs, perform the urinalysis, and enter all data into the electronic record system.
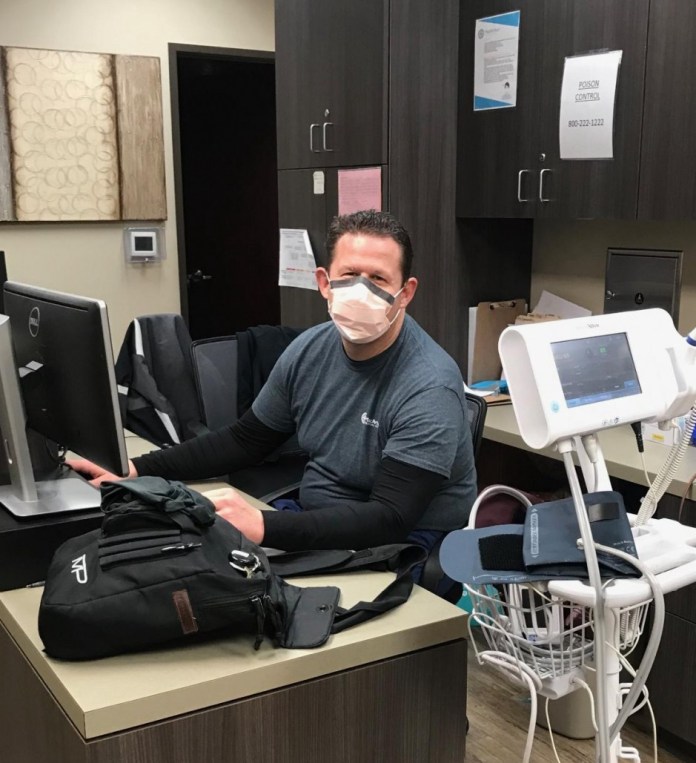
Health technology helped us manage the crisis.
While sometimes challenging, the rise of technology in healthcare helped our practice manage through the challenges. Expanded Telemedicine services allowed us to continue to see patients when they could not safely come into the office.
Some providers called patients from their homes or hotel rooms as they struggled with the same power and water issues as the rest of the community. Despite the challenges, we completed 352 virtual visits.
Crisis communication is critical.
During a crisis, the mission is simple: organize, prioritize, plan, and execute. Unexpected challenged can bring down companies and paralyze leaders. Situational threats may leave teammates feeling overwhelmed.
The Operations Team and Clinical Team met virtually at 6 am and ended their days closer to midnight as they finalized provider, staff, and patient communications and contingency care plans. We needed to know which staff members had power, water, and safe transportation.
Multiple communications went out throughout each day to keep all team members up to date with the rapidly changing situation. Everyone knew what to do and where they could best help.

Here comes the sun
By Saturday, the temperatures rose, and the sun came shining through. Most of our staff had power. Many still lacked water. We had accomplished the most important goal — we provided safe and effective care for our patients under challenging circumstances.
As we approach the one-year mark of the pandemic onset, I reflect on the past year. There is no other way to say it; it has been a difficult year to be a healthcare provider.
Despite Covid-19 and Texas Winter Storms, it feels really good knowing that careful, diligent planning and the ability to change directions and innovate is what has kept our team operational.
We are getting through it together.



